Wellness insights
Mental health in the workplace
Introduction
According to the World Health Organization, around 450 million people currently struggle with mental illness making it the leading cause of disability worldwide1. Closer to home, more than 6.7 million Canadians are affected. In fact, one in two Canadians have, or have had, a mental illness by the time they reach 40 years of age1. The cost to our economy is an estimated $51 billion a year1 . These numbers predate the devastating mental health impacts of COVID-19.
Now more than ever individuals, communities and organizations are looking for ways to prevent, manage and treat mental illness. This paper will explore the impacts of mental health in the workplace pre and post COVID-19, discuss how organizations can support their employees’ well-being and look at current available mental health resources.
Mental health versus mental illness
Mental illness and mental health are not the same—though they are often used interchangeably. While interrelated, they are distinct concepts (fig.1).
| Mental health | Mental illness |
|---|---|
| Well-being | Mental disorder |
| Mental wellness | Mental health problems/challenges |
| Emotional health | Emotional problems/challenges |
| Social/emotional wellbeing | Mental ill-health |
| Psychiatric illness |
Mental health is our state of emotional health, a sense of well-being. The World Health Organization states—if you have a brain, you have mental health. Most individuals will have mental health concerns from time-to-time such as undue stress, feelings of isolation or loneliness or simply feeling low. A mental health concern becomes a mental illness when ongoing signs and symptoms cause frequent stress and affect an individual’s ability to function.
Mental illness can be defined as changes to a person’s thoughts, moods, feelings and behaviours that cause distress or reduce a person’s ability to function. Signs and symptoms can present differently from person to person and may depend on genetics, the type of mental illness and the person’s environment. Mental illness encompasses a range of conditions including depression, anxiety, addiction, bipolar disorder, eating disorders and many others.
Mental health data
Mental health overview
Looked at in terms of economics alone, the cost of the mental health crisis is staggering. As noted, the estimated economic cost of mental health issues in Canada is at least $51 billion per year with direct costs related to health care, social services and income support making up the largest proportion1 . An estimated $20 billion of this cost stems from the workplace alone. By 2041, it is estimated that the cumulative cost of poor mental health to the Canadian economy will exceed $2.5 trillion2.
If the economic costs are upsetting, the human costs are even greater.
One in five Canadians suffer from mental illness each year1
35 per cent of Canadians are at high risk for mental illness1
Nine per cent of Canadians are taking an antidepressant1
Suicide is among the leading causes of death in Canada with an average of approximately 4,000 Canadians die by suicide every year1
Workplace and mental health prior to COVID-19
Before COVID-19, workplace mental health was one of the most important issues facing organizations. Around 500,000 Canadians in any given week are unable to work due to mental illness1. In total, the loss of productivity at work due to mental illness related absenteeism and presenteeism (working while unwell) adds up to CA$6.3 billion annually across Canada3.
- People in their early and prime working years are among the hardest hit by mental health problems and illnesses2. In fact, 21 per cent of the working population in Canada is currently experiencing mental illness4.
- Nearly half of employed Canadians with a mental health-related disability feel that one or more of their conditions makes it difficult to change or advance in their job5.
- Mental illness is a leading cause of disability in Canada1.
The costs associated with poor mental health include not just the cost of treating mental illness through medication and therapy, but also the costs incurred when poor mental health exacerbates the negative impacts and health care costs of other chronic illnesses. Mental illness can contribute to physical health issues.
- Long-term stress increases the risk of developing coronary heart disease by 150 per cent6.
- There is an association between a wide range of mental disorders and adult onset asthma and stomach ulcers6.
- Research suggests that psychosocial factors play an important role in the development of hypertension6.
Mental health and COVID-19
If Canada was already in the midst of a mental health crisis prior to COVID-19, the pandemic has increased the problem. According to a Leger poll, 40 per cent of Canadians say that their mental health is worse compared to pre-pandemic times7. As of January 2021, only 34 per cent of Canadians assessed their mental health state as excellent or very good.
- 24.3 per cent of Canadians have experienced moderate to severe anxiety8.
- 25.7 per cent of Canadians reported binge drinking8.
- 23.3 per cent of Canadians have experienced loneliness8.
- 21.7 per cent of Canadians have felt depressed8.
Albertans in particular are struggling, likely due to the combined impact of the pandemic and economic situation. This is typical and consistent with the effects seen during previous health or economic crises. According to a study by the University of Calgary, every one per cent increase in unemployment represents a 2.8 per cent increase in the province’s suicide rate9. A recent study by the Canadian Mental Health Association found that 42 per cent of Albertans are worried about their mental health during the pandemic and that 25 per cent of Albertans rated their mental health as bad or very bad10.
Unsurprisingly, these psychological impacts carry into the workforce. According to the January 2021 Mental Health Index, the entire working population is as distressed as the most distressed one per cent of working Canadians, prior to 202011. Nearly one-quarter of Canadians have considered leaving their current job due to their employer’s response to COVID-19. The most reported reason for considering leaving is increased mental stress and strain at work (53 per cent)11.
Alberta Blue Cross®
Changes in mental health and psychological trends can significantly influence utilization of health benefits. Because of this, benefit utilization tracking can provide key insights and understanding of emerging issues. As one of the largest providers of health benefits in Alberta, Alberta Blue Cross is in a unique position to assess mental health trends.
This paper will look at a few key areas of benefit utilization and how they reflect mental health trends pre- and post-COVID-19: drug, psychology, Employee Family Assistance Program (EFAP) and disability.
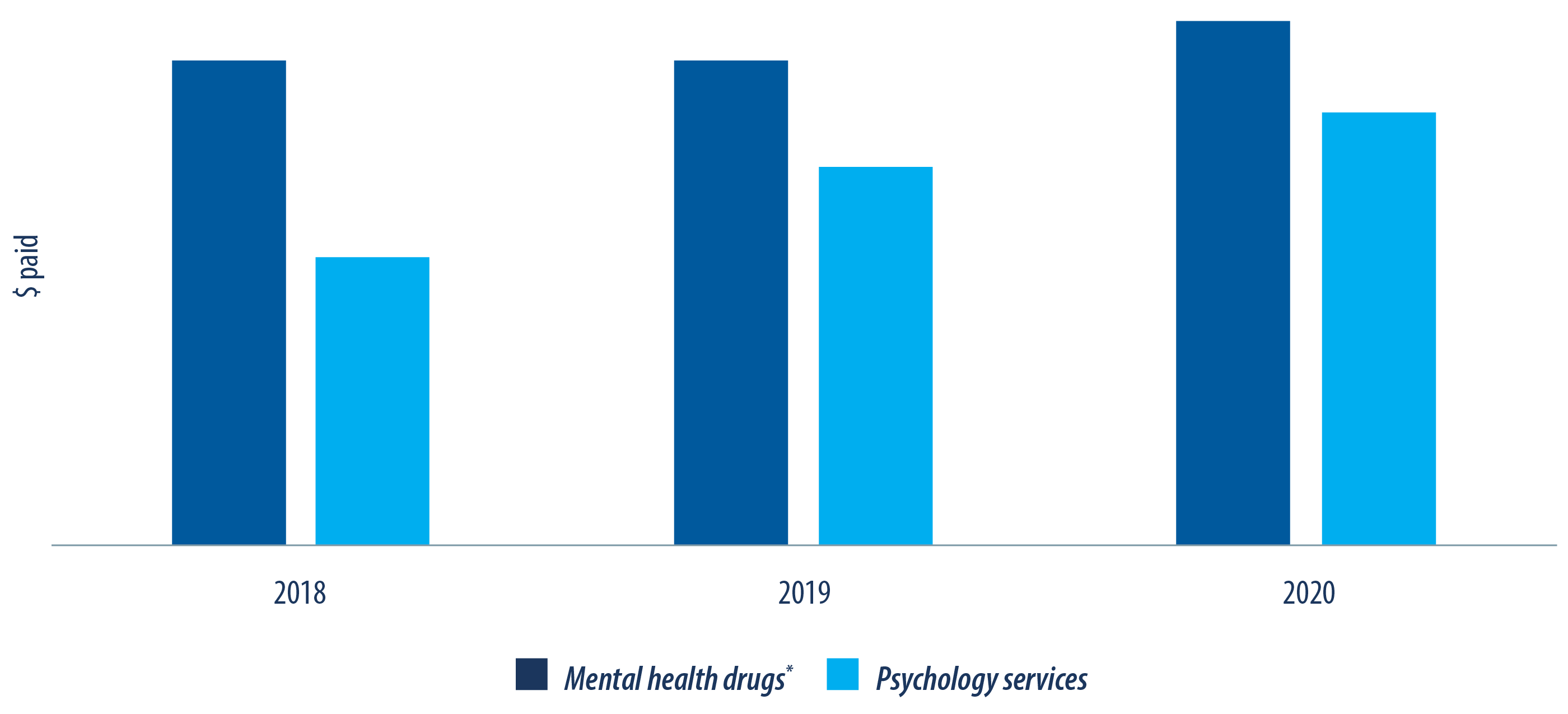
Even prior to the pandemic, we saw a consistent increase in plan utilization for mental health drug and psychology services (fig.2). The growth in mental health benefit utilization is due to both an increase in claimants and claims. The increase in mental health utilization can be attributed to multiple factors including the growing awareness of mental health and the shedding of stigma. More people feel comfortable seeking help and mental health issues are now being screened and diagnosed much more readily. In 2020, additional factors contributed to the increased utilization of mental health benefits as levels of stress and anxieties escalated with COVID-19. In addition, the previous economic downturn and recession in Alberta along with the pandemic, forced many companies to downsize, restructure or close permanently, causing significant financial stress to many Albertans.
For prescription drug utilization, mental health, as a whole, has consistently been within the top medical conditions, impacting approximately one in four claimants—which, for comparison, is roughly the same as cardiovascular drugs. We anticipate this trend to continue as mental health conditions, such as depression, are often chronic requiring long-term treatment.
*Mental health drugs include those used for depression, sleep disorder, anxiety, psychotic disorders, narcolepsy, bipolar disorder and opioid/alcohol dependence.
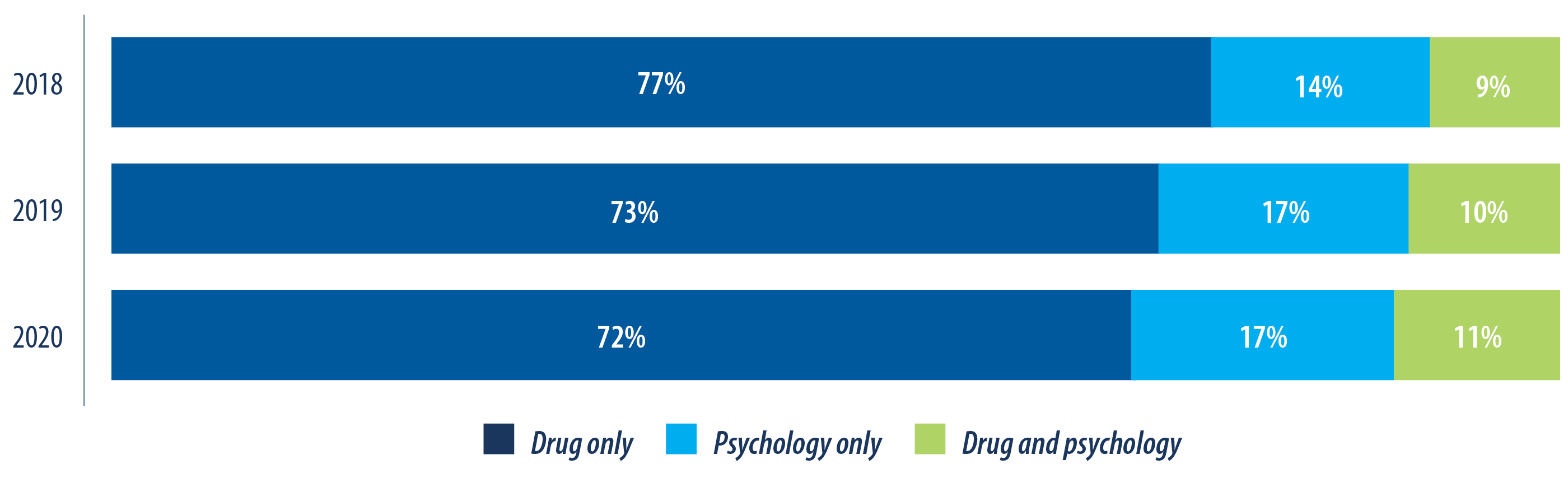
Once diagnosed, mental health conditions can be treated several ways. The most common treatments are medication and psychology services. While treatment guidelines recommend psychology and cognitive behaviour therapy as first-line treatment for depression and anxiety, the majority of mental health claimants are seeking drug treatment only (fig.3). Historically, there has been a gap in utilization between mental health drugs and psychology services, but as awareness around mental health and the benefits of psychology treatment grow, this gap is closing.
In 2020, only 11 per cent of claimants utilized both drug and psychology benefits even though it is the most effective approach. While adoption of psychology or combined treatment is slow, it is expected that utilization will continue to grow as
- mental health awareness increases—especially in the younger demographic and
- more plan sponsors modernize the psychology benefit through increased level of maximums, expanded list of eligible practitioner types, and increased access to digital assisted services like iCBT.
In fact, according to a recent survey from the Conference Board of Canada, 18 per cent of Canadian employers have raised benefit maximums since the pandemic began12. This is good news for employers as the benefits of access to psychology treatment are significant (fig. 4)

Source: Benefits Canada; Mental Health Commission of Canada
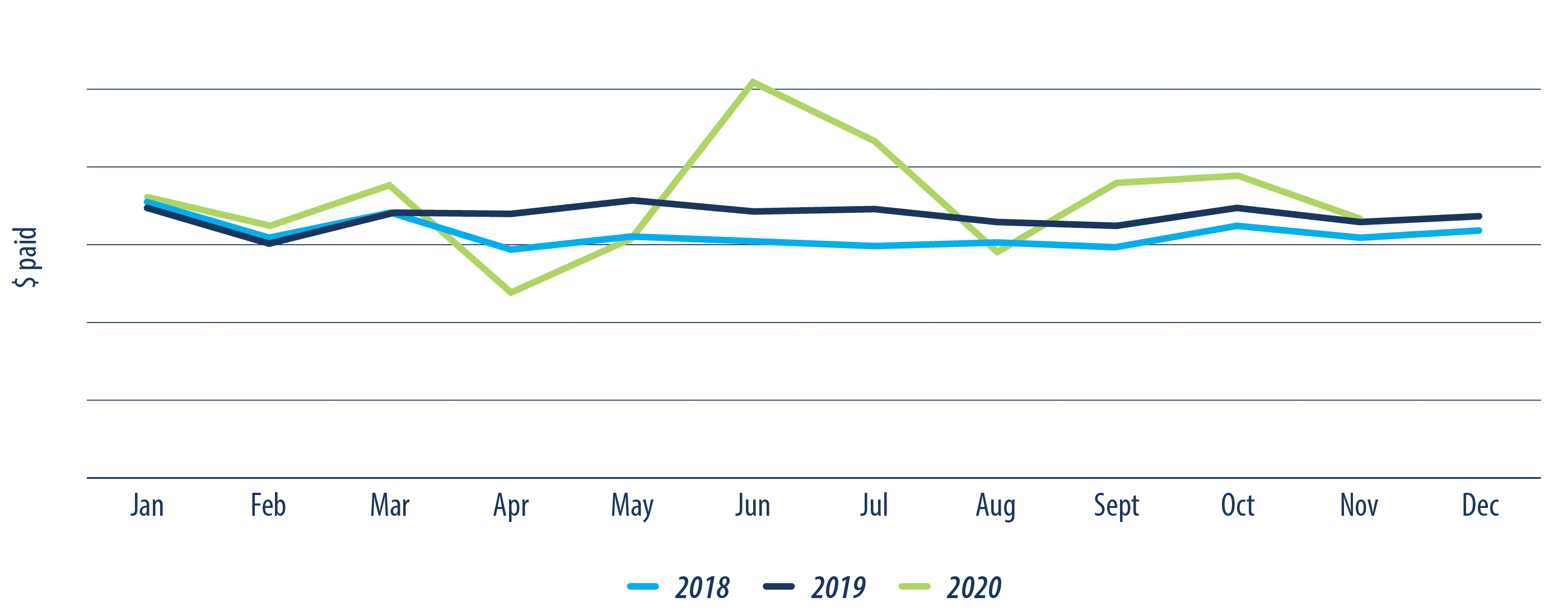
Both 2018 and 2019 follow a very similar trend line with little variation in mental health drug utilization from month-to-month (fig.5). The year 2020 starts to follow the same trend line as previous years but as soon as the COVID-19 pandemic hit Canada in March, we start to see large variability in claiming patterns.
When the pandemic hit, there was an increased demand for prescription medications due to patients requesting early refills and stockpiling. The increased demand, in combination with drug shortages and disruptions in global supply chains, led to a national recommendation to implement a 30-day supply maximum for all prescription drugs. This was implemented in Alberta on March 17, resulting in the visible drop in drug utilization. Albertans were limited to smaller refills and due to the lockdown, there were less prescriptions as people were not able to access their doctor as readily.
The plunge was short-lived as the 30-day supply limit was lifted on June 15 and people were able to fill a regular three-month supply. This is followed by a subsequent drop in July and August as the majority refilled a 3-month supply and didn’t have to return to the pharmacy as soon.
*Mental health drugs include those used for depression, sleep disorder, anxiety, psychotic disorders, narcolepsy, bipolar disorder and opioid/alcohol dependence.
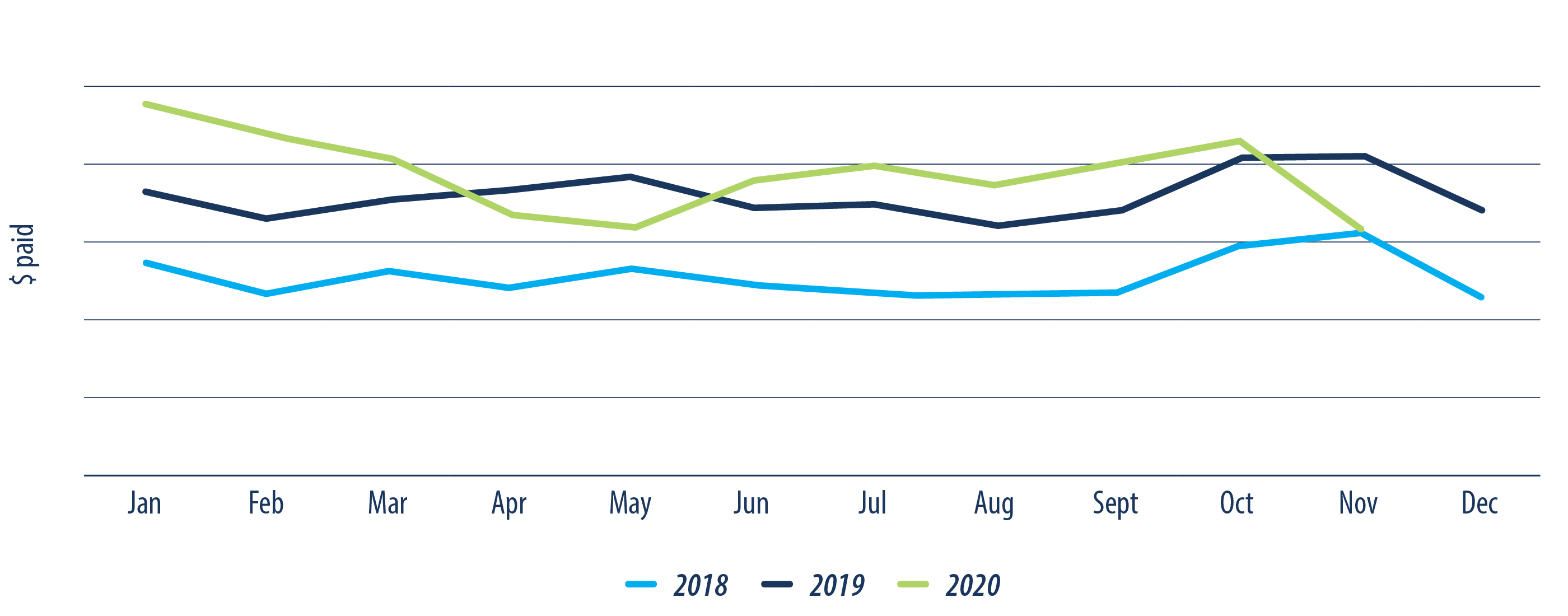
Psychology services have proven to be effective and research conducted over many years has shown significant benefits for 75 to 80 per cent of people treated. In fact, psychology benefits have the highest rate of increase compared to other extended health services (fig. 6).
Growth patterns were similar for 2018 and 2019 with certain months sharing the same fluctuations in utilization. Peaks during the months of January, May, October, November and December are typical. The slower growth in 2020 was due to the COVID-19 crisis as social distancing, financial pressures and loss of employment impacted individuals ability to access psychology services. According to a survey from the Canadian Psychological Association, with financial pressures, almost 80 per cent of respondents found that the cost of psychology services is a significant barrier in accessing care13. Despite this, total utilization was still higher compared to the previous years.
Employee and family assistance program (EFAP)
When personal problems spill over into the workforce, the result can be low productivity, absenteeism, accidents and injuries. An estimated 68 per cent of all employees will, at some time, experience problems so severe they struggle and fail to cope with day‐to‐day duties5. EFAP is a benefit that provides employees access to a variety of off-site, confidential, voluntary, short-term counselling services.
The Alberta Blue Cross EFAP is offered in tandem with extended health benefits and supplements coverage for psychology services. The EFAP program offers a wide range of services, including short-term counselling, Life Smart coaching services and an online library of interactive and assessment tools. Research has shown that EFAPs contribute to improved productivity and reduced absenteeism by addressing and improving mental health symptoms14.
In terms of type of claims made through EFAP, 86 per cent of Alberta Blue Cross claims were for counselling with the remaining 14 per cent for Life Smart services (fig.7). Of the counselling sought, the majority was for psychology at 61 per cent with anxiety, stress, and depression as the top three cases. The remaining was divided between relationship or marital, family, work, crisis or trauma, social and addiction in descending order. Around 58 per cent of the counselling was delivered by phone, while 23 per cent was face-to-face and 19 per cent on web platforms. Other mental health related conditions were anger, life transition, post trauma, eating disorders and behavioural problems.
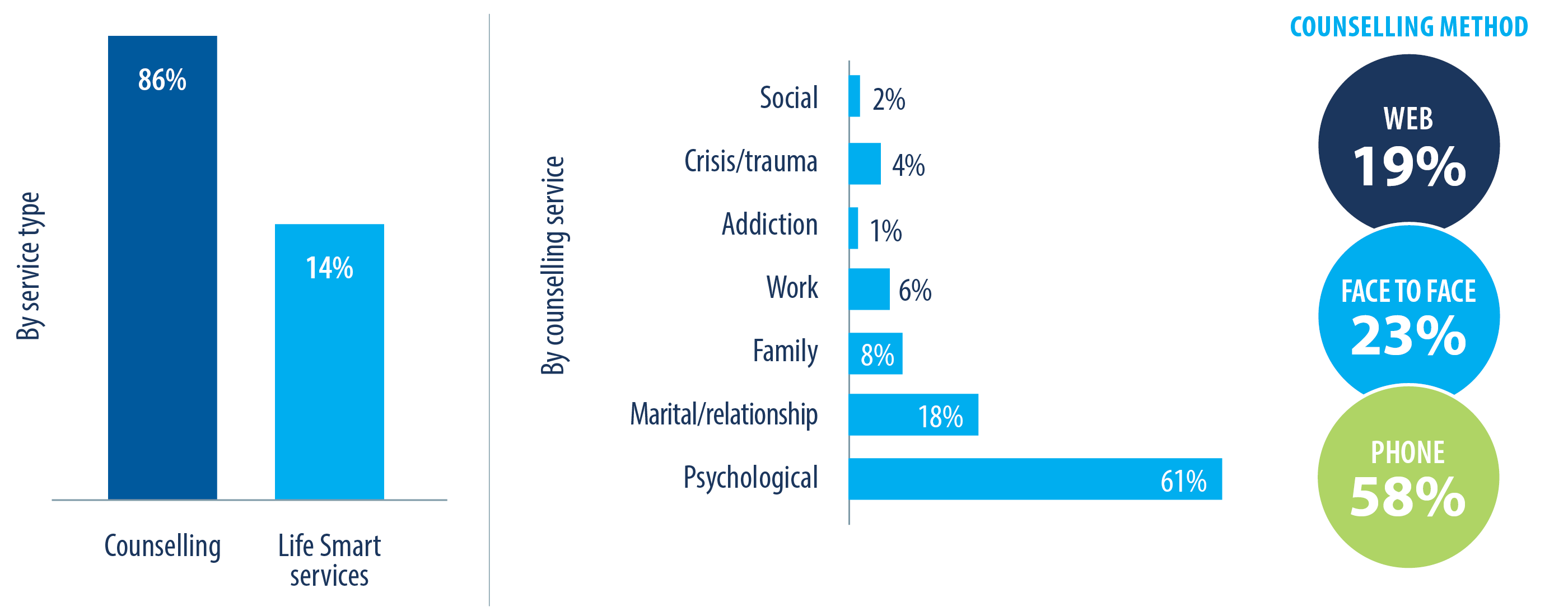
EFAP provides more than counselling services. It is also used for any issue that can escalate to affect physical, financial and social wellness with the understanding that good mental health is best achieved when all aspects of an individual’s life are in balance.
Included in the counselling are telephonic coaching services available to address topics such as childcare, eldercare, new parenting, legal advisory, financial advisory, career planning, retirement planning, nutrition, shift worker support and smoking cessation (fig.8).
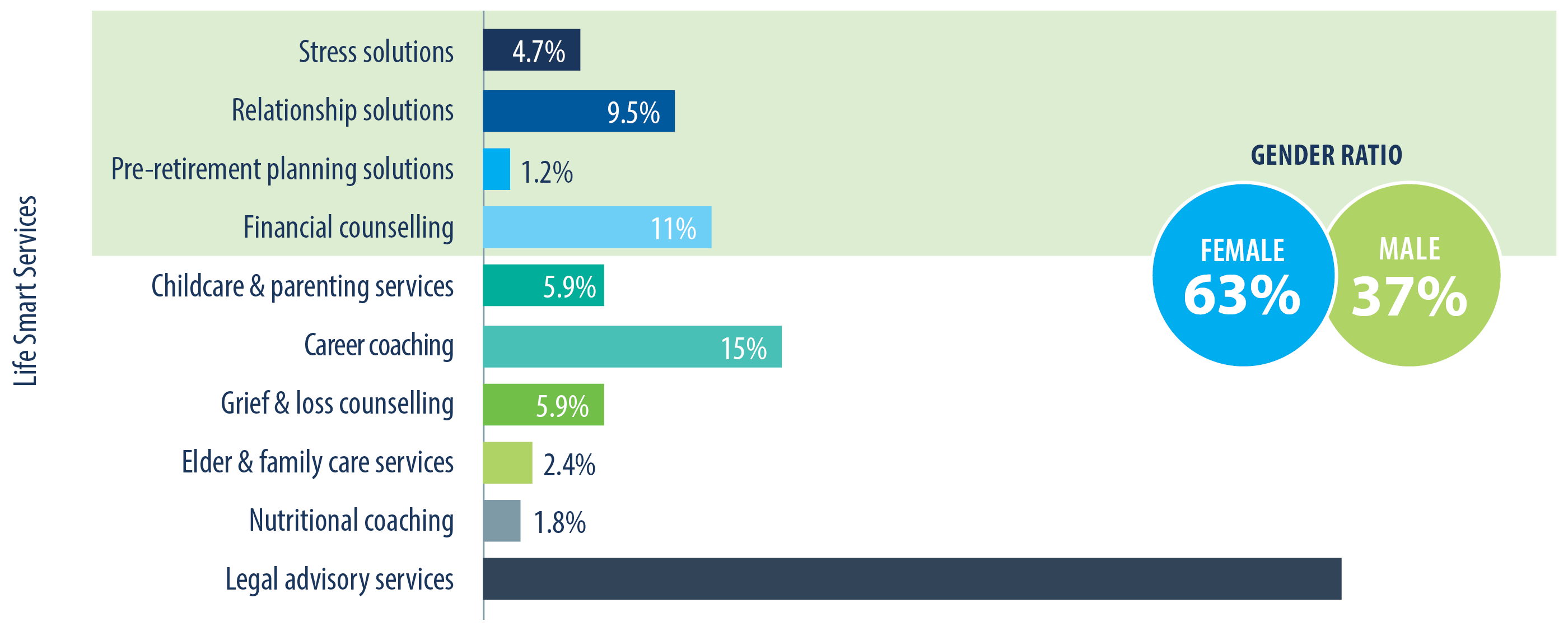
EFAPs have been around for several decades and continue to evolve to meet changing needs. Like psychology benefits, this has encouraged higher usage of services.
As indicated in the chart below, growth in utilization has been significant since 2019 where there was an initial decrease due to the economic downturn and job losses in 2019 (fig.9). There were fewer plan members eligible for coverage compared to 2018. In 2020, the total number of claims grew by 22 per cent with more employers adding EFAP coverage to supplement mental health drug and psychology coverage. EFAP is intended to be for short-term focused solutions, for individuals with long-term mental health issues referrals are made by the EFAP provider.
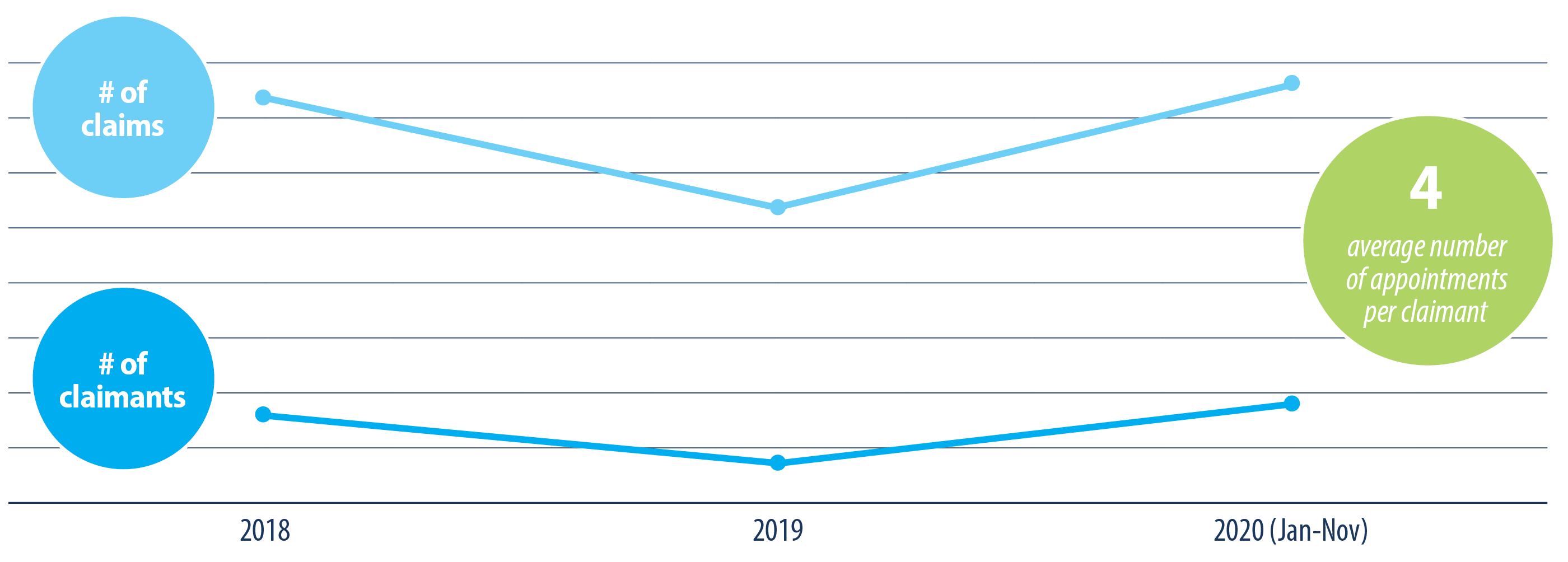
As individuals continue to face the stress and anxiety of COVID-19, utilization is likely to remain steady or increase. This may be tempered by the economic downturn and subsequent job loss and business failures.
Short-term disability and long-term disability
Over two million Canadians aged 15 or older have a mental health related disability. Mental health problems and illnesses account for approximately 30 per cent of Short-Term Disability and Long-Term Disability claims and are rated one of the top three drivers of such claims by more than 80 per cent of Canadian employers2.
According to Alberta Blue Cross utilization, mental health is the leading cause for Long-Term Disability surpassing even Musculoskeletal by more than 10 per cent (fig.10). There are a number of factors for this including the increased number of individuals suffering a mental health issue, the willingness of these individuals to disclose their mental health issues and better diagnosis by practitioners.
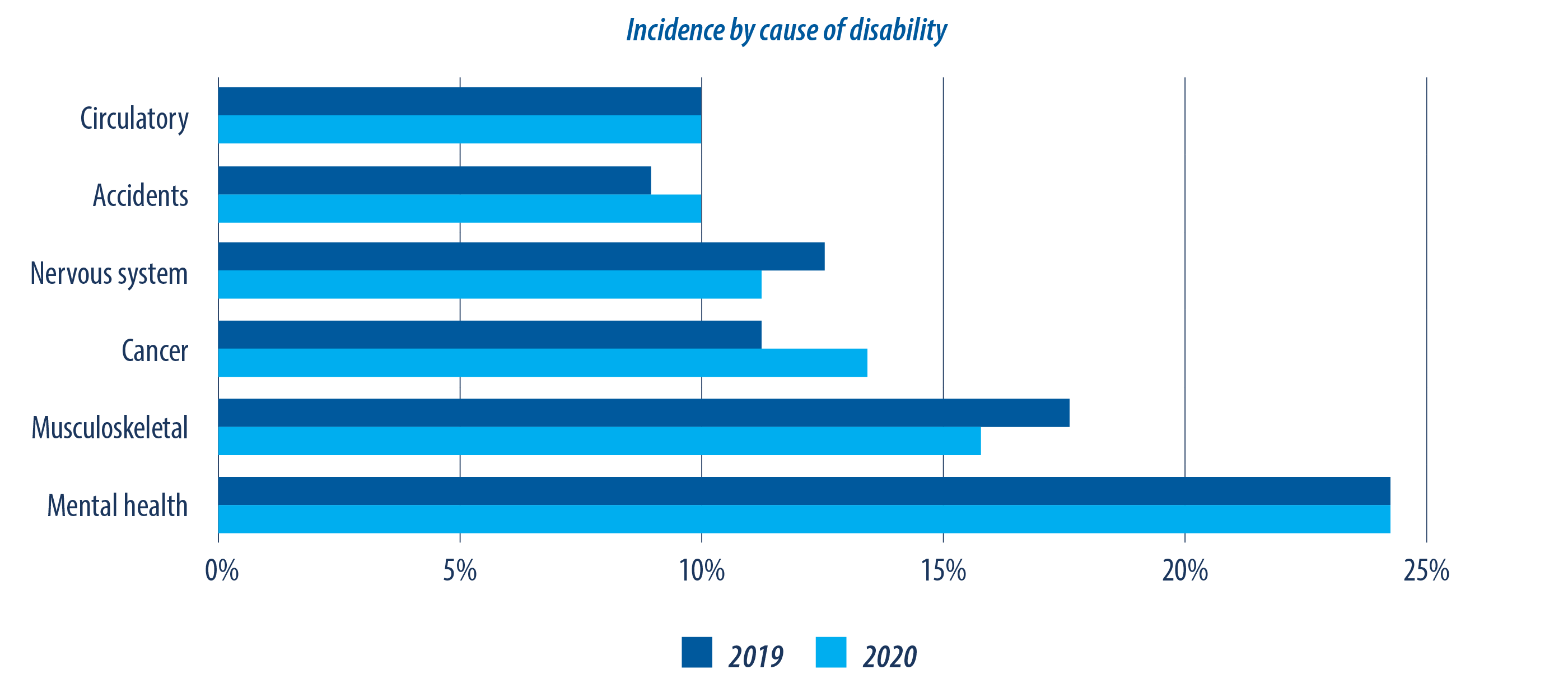
The graph below shows how the cause of disability has shifted over the past five years (fig.11). Again, this is partly due to the growing mental health crisis, but also due to decreased stigma, willingness to report and better diagnosis which is a positive step towards addressing the issue.
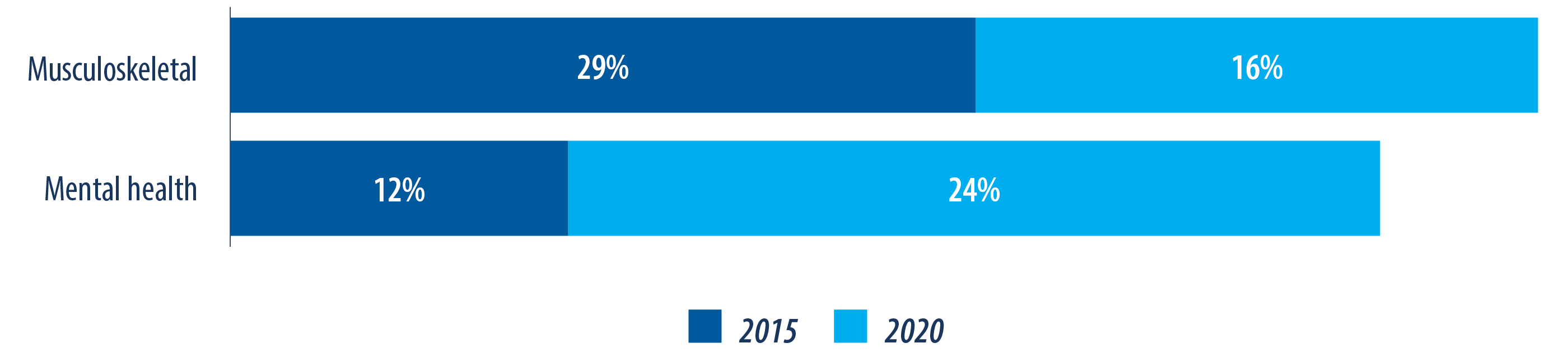
Complicating the mental health issue is that mental illness is often compounded by other health issues. In fact, four in five Canadians with a mental health related disability also have at least one other type of disability5. A total of 63 per cent of those with a mental health related disability also have a pain-related disability5 . Mental and physical health are linked. People with a long-term medical condition, such as chronic pain, are much more likely to also experience mood disorders. Conversely, people with a mood disorder are at much higher risk of developing a long-term medical condition that may prevent them from working1.
If it is possible to sum up the data into one, clear finding it is this—workplace mental health is one of the most important issues facing organizations today.
The question is, where do we go from here?
Moving forward
As employers look for ways to adapt their wellness offerings in the coming years, there are many upstream approaches organizations can take as they navigate their way through the pandemic and beyond. Research and guidelines are pushing plan advisors and human resources leaders to include broader wellness programs into their workforce strategies and plan sponsors and employers should work with their benefits advisor or provider to develop tailored and personalized strategies based on claims data and employee input and needs15.
| Taking a holistic approach to employee wellness | Mental health |
|---|---|
|
|
From treatment to prevention
With COVID-19, there is now also an increased focus on employee well-being and the understanding that wellness strategies need to expand to include a broader definition of what wellness means. They need to go beyond traditional physical fitness and occupational health and safety and become more comprehensive to include mental, physical, social, financial and now even environmental wellness. Programs need to embrace the benefits from physical fitness, proper nutrition, mental resiliency, social connections, financial supports and environmental health and their protective role in promoting positive mental health rather than rely on treatments like prescriptions or psychology services alone.
Mental health at work
Experiences of mental health and mental illness are not static but fluid and modifiable and occur over a spectrum as illustrated below.

Given that an average Canadian worker spends 30 to 40 hours per week at work, the workplace is often one of the first places symptoms of declining mental health are made evident through changes in an employee’s attitude, work habits or performance. Other changes indicating a worsening problem include
- physical changes (fatigue, low activity, sleep difficulties);
- changes in attitude, personality or behaviour (lack of interest, listless, anger); and
- changes in substance use (alcohol, nicotine).
Every person falls somewhere on the spectrum from healthy to ill (fig.12). Where an individual falls will impact the type and intensity of support they require to maintain, or reclaim, their good mental health. The important point to remember is that mental health is fluid and an individual may move left or right on the spectrum depending on many factors. However, an individual with deteriorating mental health is unlikely to recover without proper intervention or treatment.
Just as mental health and wellness works on the continuum, so does treatment of mental illness. The left, or green, portion of the continuum represents tools and supports aligned with prevention (fig.12). It then moves toward the yellow/orange which would indicate first line treatments, such as counselling. The far right, or red, represents the typical traditional treatment model, such as medication and psychology services. Ideally, treatment will begin towards the green end and individuals can avoid movement along the continuum. This is more sustainable for both the patient and health care as it leaves more acute and costly treatments available if conditions worsen. Unfortunately, prescription medication is often the default first line of treatment.
The first help individuals seek when suffering mental health symptoms is generally through a family physician and as such, treatment often starts with prescription medication. Up to 80 per cent of Canadians rely on their family physicians to meet their mental health care needs10. Over one million Canadians with a mental healthrelated disability said they require counselling services from a psychologist, psychiatrist, psychotherapist or social worker6 . An average of 52 per cent of these individuals reported receiving some counselling but needing more and almost 30 per cent reported needing counselling but receiving none6 . Barriers to accessing mental health support include
- long wait times for primary and/or psychiatric care,
- not knowing where to get help,
- shortage of accessible mental health professionals, and
- cost of services not covered by private insurance plans.
Mental health supports
The following chart shows available mental health tools and treatments within the mental health spectrum (fig.13). Traditionally, employers have supported employees’ mental health towards the red, or treatment, side by providing employer benefits that cover the costs of prescription drugs and psychology treatment. We are, however, seeing more employers enhancing their psychology benefit, adding EFAP and other alternatives to their coverage as demand and awareness grows. As mentioned earlier, psychology benefit has the highest rate of increase compared to other extended health benefits. As well, options like Health Spending Accounts (HSA) and Wellness Spending Accounts (WSA) allow employees to access the tools and treatments that best fit their mental health needs at any given time. Workplaces are also ideally situated to support and promote prevention.
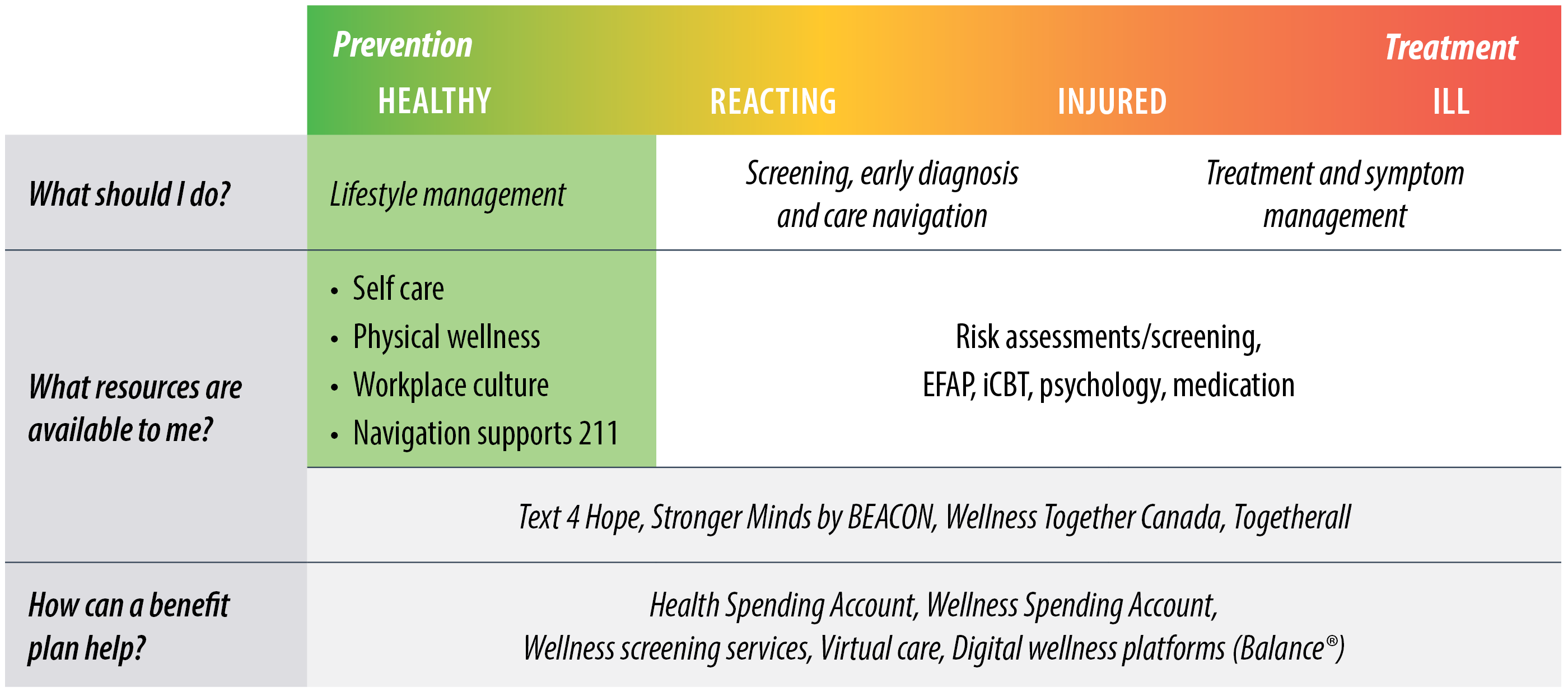

Workplaces can play an essential part in maintaining positive mental health. They provide opportunities to feel productive, chances to connect and socialize with others and can support individuals in developing new skills and experiences. Workplaces can also be stressful environments that contribute to the rise of mental health problems and illnesses. That’s why organizations need to move from a treatment to prevention model and take a holistic approach to employee wellness.
Steps to success
If you are looking to begin or adapt your existing employee wellness programs, following these initial steps can set you up for success.
- Invest in proactive programs that promote positive mental health in addition to treatment—this means going beyond delivering interventions for poor mental health to promoting positive mental health through lifestyle management behaviors.
- Prioritize investments in the highest-impact areas, such as leadership training and return-to-work programs demonstrating your leadership commitment and positive wellness culture.
- Track key performance indicators and calculate return on investment to demonstrate the financial and nonfinancial benefits of mental health programs such as employee engagement, decreased absenteeism, and productivity
- Use data analytics to evaluate whether investments are having the desired impact and adoption rate and adapt programs based on the flexible needs of your employees.
Post pandemic considerations
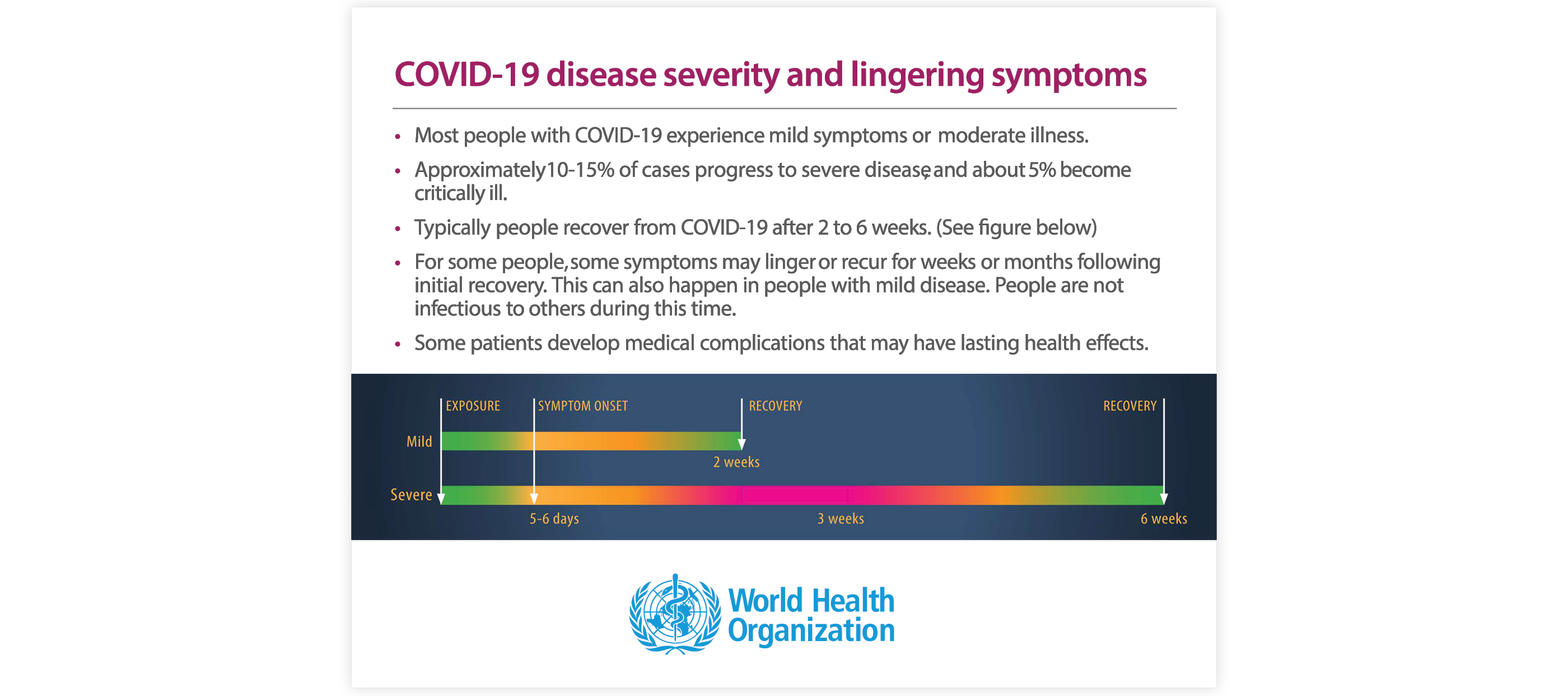
Though the long-term effects of COVID-19 are just beginning to make themselves known, it is safe to say that communities, health care systems and organizations will be coping with them for years to come (fig.14)
Front line and essential workers dealing with the immediate and unimaginable realities of the pandemic may be at increased risk for severe mental health difficulties associated with stress and trauma. People already dealing with mental illness are at risk for increased deterioration of their mental well-being and increased symptoms. Survivors of COVID-19 may experience lingering effects and symptoms or develop medical complications that have lasting effects. They may also suffer long lasting mental health deterioration.
As we move further into the recovery phase of COVID-19, we cannot let feelings of relief divert attention from those who will require longer term care and support. Post COVID-19 is full of the unknown and like other global events, it has changed our world. It will be important to carefully study and research the mid- to long-term effects and continue to push towards embracing preventative approaches to addressing mental illness.
Conclusion
450 million people currently struggle with mental illness worldwide making this one of the most pressing issues facing nations, governments, organizations and communities today. With current global issues, including COVID-19, it is unlikely that those numbers will decrease if left unaddressed. It is time to look at how and where we can best meet the needs of those struggling with issues. Prevention and earlier access to support is key. With 66 per cent of Canadians being part of the workforce, workplaces have tremendous potential to help impact the mental health crisis16. Building positive workplace culture that promotes mental health support through prevention, training and benefits not only helps employees but can significantly help an organization’s bottom line.
Questions
If you would like to further discuss the information in this report or how Alberta Blue Cross can support your organizational mental health, please reach out to wellness@ab.bluecross.ca.
References
[1] https://www.camh.ca/en/driving-change/the-crisis-is-real/mental-health-statistics
[3] https://cmha.ca/fast-facts-about-mental-illness
[4] http://ccohs.ca/
[5] https://www150.statcan.gc.ca/n1/pub/11-627-m/11-627-m2019005-eng.htm
[6] https://www.workplacestrategiesformentalhealth.com/resources/psychological-health-and-safety-statist
[7] https://leger360.com/surveys/one-year-anniversary-of-covid-19-in-canada-survey/
[8] https://www.camh.ca/en/health-info/mental-health-and-covid-19/covid-19-national-survey
[12] https://www.conferenceboard.ca/in-fact/working-through-covid-19-employee-benefits/
[13] https://cpa.ca/docs/File/Media/Alta%20Access%20to%20Services%20CPA%20CPAP%20Nanos%20Survey.pdf
[14] https://www.ab.bluecross.ca/employer-groups/employee-assistance.php
[16] https://www150.statcan.gc.ca/n1/pub/75-006-x/2019001/article/00004-eng.htm